Internal mini form
Contact Us Today
Reaching the expected developmental benchmarks of infancy and childhood – sitting, rolling over, crawling, standing and walking – are a matter of great joy for parents, but what if a child’s developmental timetable seems delayed? There are many tell-tale signs that a child may have Cerebral Palsy, but those factors can be indicative of many conditions.
Signs and symptoms of Cerebral Palsy
Signs of Cerebral Palsy are different from symptoms of Cerebral Palsy.
Signs are clinically identifiable effects of brain injury or malformation that cause Cerebral Palsy. A doctor will discern signs of a health concern during the exam and testing.
Symptoms, on the other hand, are effects the child feels or expresses; symptoms are not necessarily visible.
Impairments resulting from Cerebral Palsy range in severity, usually in correlation with the degree of injury to the brain. Because Cerebral Palsy is a group of conditions, signs and symptoms vary from one individual to the next.
The primary effect of Cerebral Palsy is impairment of muscle tone, gross and fine motor functions, balance, control, coordination, reflexes, and posture. Oral motor dysfunction, such as swallowing and feeding difficulties, speech impairment, and poor facial muscle tone can also indicate Cerebral Palsy.
Associative conditions, such as sensory impairment, seizures, and learning disabilities that are not a result of the same brain injury, occur frequently with Cerebral Palsy. When present, these associative conditions may contribute to a clinical diagnosis of Cerebral Palsy.
Many signs and symptoms are not readily visible at birth, except in some severe cases, and may appear within the first three to five years of life as the brain and child develop.
In these instances, the most apparent early sign of Cerebral Palsy is developmental delay. Delays in reaching key growth milestones, such as rolling over, sitting, crawling and walking are cause for concern. Practitioners will also look for signs such as abnormal muscle tone, unusual posture, persistent infant reflexes, and early development of hand preference.
If the delivery was traumatic, or if significant risk factors were encountered during pregnancy or birth, doctors may suspect Cerebral Palsy immediately. In moderate to mild cases of Cerebral Palsy, parents are often first to notice if the child doesn’t appear to be developing on schedule. If parents do begin to suspect Cerebral Palsy, they will likely want to ask their physician to evaluate their child for Cerebral Palsy.
Most experts agree; the earlier a Cerebral Palsy diagnosis can be made, the better.
However, some caution against making a diagnosis too early, and warn that other conditions need to be ruled out first. Because Cerebral Palsy is the result of brain injury, and because the brain continues to develop during the first years of life, early tests may not detect the condition. Later, however, the same test may, in fact, reveal the issue.
The earlier a diagnosis is made, the sooner a child can be enrolled in early intervention programs and treatment protocols. Early interventions and therapies have proven to help a child maximize their future potential. Early diagnosis also helps families qualify for government benefit programs to pay for such measures.
Eight clinical signs of Cerebral Palsy
Since Cerebral Palsy is most often diagnosed in the first several years of life, when a child is too young to effectively communicate his or her symptoms, signs are the primary method of recognizing the likelihood of Cerebral Palsy.
Cerebral Palsy is a neurological condition which primarily causes orthopedic impairment. Cerebral Palsy is caused by a brain injury or brain abnormality that interferes with the brain cells responsible for controlling muscle tone, strength, and coordination. As a child grows, these changes affect skeletal and joint development, which may lead to impairment and possibly deformities.
The eight clinical signs include muscle tone, movement coordination and control, reflexes, posture, balance, gross motor function, fine motor function and oral motor function. These are detailed below.

The most noticeable sign of Cerebral Palsy is impairment of muscle tone – the ability of muscles to work together by maintaining proper resistance. Muscles coordinate with other muscles, oftentimes in pairs. As some muscles contract, others must relax. Even something as simple as sitting requires coordination of many muscles; some flexing while others relax. The brain injury or malformation that caused Cerebral Palsy impairs the ability of the central nervous system to coordinate muscle movement.
Muscle Tone
Proper muscle tone allows limbs to bend and contract without difficulty, enabling an individual to sit, stand, and maintain posture without assistance. Improper muscle tone occurs when muscles do not coordinate together.
When this happens, those muscles that work in pairs – biceps and triceps, for example – may both contract or relax at the same time, impeding movement and coordination. Trunk muscles might relax too much, making it difficult to maintain a tight core; this can result in impaired posture and an inability to sit or to move from a sitting to standing position.
A child with Cerebral Palsy may demonstrate any combination of these signs. Different limbs may be affected by different impairments. The two most common signs of abnormal muscle tone are hypotonia and hypertonia, but tone can be defined in other ways as well:
- Hypotonia – decreased muscle tone or tension (flaccid, relaxed, or floppy limbs)
- Hypertonia – increased muscle tone or tension (stiff or rigid limbs)
- Dystonia – fluctuating muscle tone or tension (too loose at times and too tight at others)
- Mixed – the trunk of the body may be hypotonic while the arms and legs are hypertonic
- Muscle spasms – sometimes painful, involuntary muscular contraction
- Fixed joints – joints that are effectively fused together preventing proper motion
- Abnormal neck or truncal tone – decreased hypotonic or increased hypertonic, depending on age and Cerebral Palsy type
- Clonus – muscular spasms with regular contractions
- Ankle/foot clonus – spasmodic abnormal movement of the foot
- Wrist clonus – spasmodic movement of the hand

The impairment of muscle tone affects a child’s limbs and body in different ways, although all children with Cerebral Palsy will likely feel some effect on muscle control and coordination. Different muscle control impairments can combine to cause limbs to be perpetually extended, contracted, constantly moving in rhythmic patterns or jerking spastically.
Movement , coordination and control
Some signs will be more apparent when the child is under stress. Some may be task related, such as reaching for an object. Sometimes signs will seem to disappear when the child is asleep and muscles are relaxed.
It is common for a child to experience different types of impaired muscle control in opposite limbs. Coordination and control can likewise be affected differently in each limb.
The impairment of coordination and control fall under the following types:
- Spastic movements – hypertonic movements where the muscles are too tight resulting in muscle spasms, scissoring of the legs, clonus, contracture, fixed joints, and over-flexed limbs
- Athetoid or dyskinetic movements – fluctuating muscle tone causing uncontrolled, sometimes slow, writhing movements which can worsen with stress
- Ataxic movements – poor coordination and balance making tasks – such as writing, brushing teeth, buttoning shirts, tying shoes, and putting keys into slots – difficult
- Mixed movements – a mixture of movement impairments, most commonly a combination of spastic and athetoid types, affecting different limbs
- Gait disturbances – control impairments affecting the way a child walks
Gait disturbances include:
- In-toeing – toes angle or rotate inward
- Out-toeing – toes angle or rotate outward
- Limping – more weight is placed on one foot than the other, causing a dipping, or wavy stride
- Toe walking – the weight is unevenly placed on the toes
- Propulsive gait – a child walks hunched over in a stiff posture with the head and shoulders bent forward
- Spastic and scissor gait – the hips flex slightly making it look like the child is crouching while knees and thighs slide past one another like scissors
- Spastic gait – one leg drags due to muscle spasticity
- Steppage gait – toes drag because the foot drags
- Waddling gait – duck-like walking pattern that can appear later in life
Reflex
Certain abnormal reflexes may also indicate Cerebral Palsy. Hyperreflexia are excessive reflex responses that cause twitching and spasticity. Underdeveloped or lacking postural and protective reflexes are warning signs for abnormal development, including Cerebral Palsy.

Reflexes are involuntary movements the body makes in response to a stimulus. Certain primitive reflexes are present at or shortly after birth, but disappear at predictable stages of development as the child grows. Specific reflexes that do not fade away – or those that don’t develop as the child grows – can be a sign of Cerebral Palsy.
Abnormal primitive reflexes may not function properly in children with Cerebral Palsy, or they may not disappear at specific points in development as they do with children with no impairment.
Common primitive reflexes that may improperly function or persist include, but are not limited to:
- Asymmetrical tonic reflex – when the head turns, the legs on the same side will extend, and the opposite limbs contract like in a fencing pose. Asymmetrical tonic reflex should disappear around six months of age.
- Symmetrical tonic neck reflex – the infant assumes a crawling position when the head is extended. Symmetrical tonic neck reflex should disappear between eight and 11 months.
- Spinal gallant reflexes – when the infant lies on its stomach, the hips will turn towards the side of the body that is touched. Spinal gallant reflexes should disappear between three and nine months.
- Tonic labyrinthine reflex – when the head is tilted back, the back arches, the legs straighten, and the arms bend. Tonic labyrinthine reflex should disappear by three-and-a-half years of age.
- Palmer grasp reflex – when stimulating the palm the hand flexes in a grasping motion. Palmer grasp reflex should disappear around four to six months.
- Placing reflex – when an infant is held upright and the back of a foot touches the surface, the legs will flex. Placing reflex should disappear by five months.
- Moro (startle) reflex – when the infant is tilted so his or her legs are above their head, the arms will extend. Moro reflex should disappear by six months.
Early hand preference can also indicate possible impairments. A child normally develops hand preference in his or her second year. As this is a wide timeframe and rough average, development of hand preference, especially if it is early preference, is cause for concern. Various sources state that early hand preference falls between 6-18 months.

Posture
Cerebral Palsy affects posture and balance. Signs may appear as an infant begins to sit up and learn to move about. Typically, posture is expected to be symmetrical. For example, a baby in a sitting position would normally have both legs in front. When bent, they become mirror images of one another.
Asymmetrical posture means the right and left limbs will not mirror one another. The hip-joints are one area where this is often prominent in instances of Cerebral Palsy. One leg will bend inward at the hip, and the other will bend outward.
Much like reflexes, postural responses are expected reactions when putting a baby in certain positions. They typically appear as the baby develops. Impairment may be a possibility if the responses do not develop, or if they are asymmetric.
Much like reflexes, postural responses are expected reactions when putting a baby in certain positions. They typically appear as the baby develops. Impairment may be a possibility if the responses do not develop, or if they are asymmetric.
Common postural responses are:
- Traction
- Landau reflex – when the infant is supported in a lying position, pushing the head down will cause the legs to drop, and lifting the head will cause them to rise. This response appears around four or five months of age.
- Parachute response – when the infant is positioned with his or her head towards the ground, the infant should instinctively reach as if bracing for impact. This response appears around eight to 10 months of age.
- Head righting – when an infant is swayed back and forth, his or her head will remain straight. This response appears around four months of age.
- Trunk righting – when a sitting infant is quickly pushed to the side, the infant will resist the force and use opposite hand and arm to brace against impact. This response appears around eight months of age.

Balance
The impairment of gross motor function can affect a child’s ability to balance. Signs become recognizable as a child learns to sit, rise from a sitting position, and begins crawling or walking. Infants need to use their hands often as they learn these skills. They develop the strength, coordination, and balance to accomplish the task when mastering it without the use of their hands.
A child’s inability to sit without support can be a sign of Cerebral Palsy. The Gross Motor Function Classification System, or GMFCS, a five-level system commonly used to classify function levels, uses balance while sitting as part of its severity level system.
Signs to look for when a child sits include:
- Requiring both hands for support
- Having difficulty balancing when not using hands for support
- Unable to sit without using hands for support
Other signs to look for include, but are not limited to:
- Swaying when standing
- Unsteady when walking
- Difficulty making quick movements
- Needing hands for activities that require balance
- Walking with abnormal gait
Balance is often the same whether a child’s eyes are open or closed. Balance impairment is most often associated with ataxic, and to a lesser degree, spastic Cerebral Palsy.
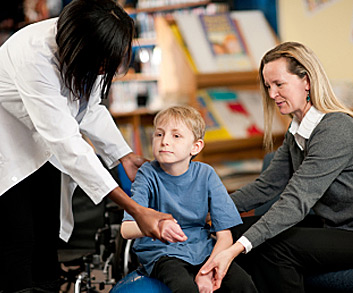
As a child develops, signs of impaired or delayed gross motor function may be noticeable. The ability to make large, coordinating movements using multiple limbs and muscle groups is considered gross motor function.
Gross motor function
Gross motor function may be impaired by abnormal muscle tone, especially hypertonia or hypotonia.
For example, hypertonic limbs can be too tight, or inflexible, to allow proper flexion and movement; whereas hypotonic limbs may be too loose to properly support a child’s movements.
As a baby’s brain and body develop, they are expected to reach developmental milestones. Reaching the milestone later than expected, or reaching it but with low quality of movement (such as favoring one side while crawling), are possible signs of Cerebral Palsy.
- Impaired gross motor functions – limited capability of accomplishing common physical skills such as walking, running, jumping, and maintaining balance.
- Delayed gross motor functions – physical skills developed later than expected; often used in conjunction with developmental milestones for predictable stages of development.
Significant milestones of gross motor function include:
- Rolling
- Sitting up
- Crawling
- Standing
- Walking
- Balancing
These should be monitored to note when the baby reaches the milestone, and the quality of movement.

Fine motor function
Executing precise movements defines the category of fine motor function. Fine motor control encompasses many activities that are learned, and involves a combination of both mental (planning and reasoning) and physical (coordination and sensation) skills to master.
Impaired or delayed fine motor skills are an indicator of possible Cerebral Palsy. Intention tremors, where a task becomes more difficult as it gets closer to completion, is one such sign.
Examples of fine motor function development are:
- Grasping small objects
- Holding objects between thumb and forefinger
- Setting objects down gently
- Using crayons
- Turning pages in a book
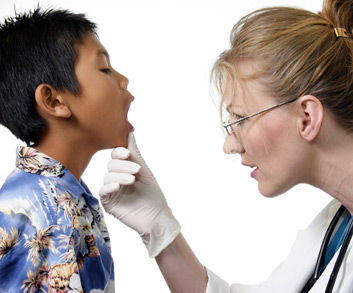
Oral motor function
Difficulty in using the lips, tongue, and jaw indicate impaired oral motor function; this is a sign that may be present in up to 90% of preschool-aged children diagnosed with Cerebral Palsy. Signs of oral motor function impairment include, but are not limited to difficulty with:
- Speaking
- Swallowing
- Feeding/chewing
- Drooling
Speech requires proper intellectual and physical development. Cerebral Palsy impairs the physical aspects of speaking by improperly controlling the muscles required to speak. Oral motor impairment can affect:
- Breathing – the lungs, and specifically the muscles controlling inhalation and exhalation necessary for proper speech patterns. The diaphragm and abdominal muscles are important for proper air flow and posture.
- Articulating – muscles controlling the face, throat, mouth, tongue, jaw, and palate all must work together to form the proper shape necessary for pronunciation of words and syllables.
- Voicing – vocal cords are controlled by muscles that essentially stretch the vocal folds between two regions of cartilage.
Apraxia, an inability of the brain to effectively transmit proper signals to the muscles used in speaking, is one type of speech impairment common to Cerebral Palsy. It is divided into two types:
- Verbal apraxia – affects the articulation muscles, especially regarding the specific sequence of movements needed to carry out proper pronunciation. It is common in children with hypotonia.
- Oral apraxia – affects the ability to make nonspeaking movements of the mouth, but is not related solely to speaking. Examples of oral apraxia would be the inability to lick the lips or inflate the cheeks.
Dysarthria is another speech impairment common to Cerebral Palsy. Like apraxia, it is a neurological impairment, as opposed to a muscular condition. It is often found in Cerebral Palsy that results in hypertonia and hypotonia. Dysarthria is broken into the following subgroups:
- Ataxic dysarthria – slow, erratic, inarticulate speech caused by poor breathing and muscular coordination
- Flaccid dysarthria – nasal, whiny, breathy speech caused by the inability of the vocal chords to open and close properly. There may be difficulty with consonants.
- Spastic dysarthria – slow, strenuous, monotone speech and difficulty with consonants
- Mixed dysarthria – all three may be present.
Drooling is another sign of Cerebral Palsy that results from muscles in the face and mouth not being able to properly control coordination. Some specific factors which can contribute to drooling are impairments in:
- Swallowing
- Closing the mouth
- Positioning the teeth
- Inability to move saliva to back of mouth
- Tongue thrusting
Feeding difficulties can be present with Cerebral Palsy. They typically manifest as decreased ability to chew and swallow, and may also involve choking, coughing, gagging, and vomiting.
RESOURCES
Signs of Cerebral Palsy
For other sources with general information on the signs and symptoms of Cerebral Palsy, MyChild™ recommends the following:
Centers for Disease Control and Prevention:
American Academy of Pediatrics Cerebral Palsy
National Dissemination Center for Children with Developmental Disabilities